

We attempt to limit the period of corticosteroid administration to 2 to 3 weeks or less but prolong the period of tapering the drug if neurologic signs return. This brief period of corticosteroid administration generally produces few adverse effects, but some patients complain of insomnia and a few will develop depressive or manic symptoms. Patients who, because of clinical relapse on withdrawal of the medication, require treatment for more than several weeks are subject to the effects of hypercortisolism, including the facial and truncal cosmetic changes of Cushing syndrome, hypertension, hyperglycemia and erratic diabetic control, osteoporosis, aseptic necrosis of the acetabulum, and cataracts; less often, there may be gastrointestinal hemorrhage and activation of tuberculosis. However, pulses of high-dose intravenous steroids, as described above, administered once each month, seem to keep some patients from having relapses and are better tolerated than the continuous administration of oral medication. It must be acknowledged that the corticosteroid regimens and dosages in common use are derived from anecdotal experience (the Optic Neuritis Treatment Trial being an exception) and that certain patients appear, at least for a period of time, to respond better to one or another method of treatment. Treatment of Optic Neuritis the Optic Neuritis Treatment Trial, reported by Beck and colleagues, cautioned against the use of oral prednisone in the treatment of acute optic neuritis (see also Lessell). In this study it was found that the use of intravenous methylprednisolone followed by oral prednisone did indeed speed the recovery from visual loss, although at 6 months there was little difference between patients treated in this way and those treated with placebo. They reported that treatment with oral prednisone alone slightly increased the risk of new episodes of optic neuritis. In a subsequent randomized trial conducted by Sellebjerg and colleagues, it was found that methylprednisolone 500 mg orally for 5 days had a beneficial effect on visual function at 1 and 3 weeks. However, at 8 weeks, no effect could be shown (compared with the placebotreated group), nor was there an effect on the subsequent relapse rate. Glatiramer acetate may be particularly useful in patients who become resistant, i. The rate of such antibody emergence varies directly with the frequency of use of interferon: after a period of years, 30 percent of patients demonstrate antibodies with daily administration, 18 percent with alternate-day use, and less than 5 percent with weekly use. More recent changes in the preparation of interferon have led to reported rates of only 2 percent with antibodies after 1 year of use. There is some evidence that the presence of these antidrug antibodies diminishes the effectiveness of interferon. Antibodies do not develop to glatiramer acetate, and this has been emphasized as a relative advantage of the latter drug. Overall, the side effects of these interferon agents are modest, consisting mainly of flu-like symptoms, sweating, and malaise beginning several hours after the injection and persisting for up to 14 h; they are reduced by nonsteroidal anti-inflammatory drugs and tend to abate with continued use of the agents. There may also be a tendency to depression in susceptible patients treated with interferon, and in our experience, this information, when openly discussed with the patient, has sometimes influenced the decision regarding choice of treatment. A rare but notable problem is the induction of a "systemic capillary leak syndrome" in patients with a monoclonal gammopathy who receive interferon. Patients receiving glatiramer acetate should be warned of an infrequent complication consisting of flushing, chest tightness, dyspnea, palpitations, and severe anxiety. Injection site reactions occur with both classes of drugs but are rarely troublesome if the sites are rotated. From these studies, the concept has emerged that subclinical lesions are of importance and that, over time, cognitive decline and neurologic deficits are more likely to occur if the rate of progression is not reduced by treatment. There are few circumstances where such treatment is mandated immediately and we allow enough time for the patient to consider the alternatives. The endless discussions about the superiority of weekly, every-other-day, or daily medications cannot be resolved except to say that more frequent administration is probably marginally better. In the case of interferon, however, it leads to a higher rate of antibody production over years. With all of these treatments it should be acknowledged that there is no certain correlation between the number of relapses and the ultimate disability despite authoritative statements to the contrary (see Confavreux et al, 2000). The need to treat patients with optic neuritis alone with interferon has not been satisfactorily resolved. We have generally avoided this approach except in a few patients with repeated episodes involving both eyes at various times. Immunosuppressive Drugs A number of agents that modify immune reactivity have been tried, with limited success. Drugs such as azathioprine and cyclophosphamide, as well as total lymphoid irradiation, have been given to small groups of patients and seem to have improved the clinical course of some (Aimard et al, Hauser et al, Cook et al).
Rarely, cataplexy precedes the advent of sleep attacks, but usually it follows them, sometimes by many years. Sleep paralysis and hypnagogic hallucinations together are stated to occur in about half the patients, but the incidence has been far less in our few personally observed cases. It should also be noted that hypnagogic paralysis and hallucinations occur occasionally in otherwise normal persons and that normal children, especially when tickled, may laugh to the point of cataplexy. The degree of sleepiness, once it has stabilized, rarely lessens, although cataplexy, sleep paralysis, and hallucinations improve or disappear with age in about one-third of patients who have those features (Billiard and Cadilhac). No other condition is consistently associated with narcolepsycataplexy and none develops later. The risk of narcolepsy in a first-degree relative of an affected individual is 1 to 2 percent, more than 25 times that in the general population. As reviewed by Chabas and colleagues, important insights into the pathogenesis have come from studies of recessively inherited narcolepsy in three species of dogs, in which mutations have been identified in a gene encoding a receptor for the protein hypocretin (Lin et al). In both humans and animals, hypocretin-containing neurons in the hypothalamus send projections widely through the brain and particularly to structures implicated in control of sleep: the locus coeruleus (noradrenergic), the tuberomammillary nucleus (histaminergic), the raphe nucleus (serotonergic), and the ventral tegmental area (dopaminergic). A number of compelling data implicate hypocretin and its receptors in human narcolepsy. First, a narcoleptic patient has been described with a mutation in the gene encoding human hypocretin. Somewhat suprisingly, several lines of evidence suggest an autoimmune causation for narcolepsy. Because the mode of inheritance of narcolepsy is not clearly mendelian (Kessler et al), it has been proposed that the disease reflects a genetic predisposition, possibly with a superimposed autoimmune reaction that impairs the function of hypocretin neuronal systems or damages the neurons that secrete the peptide. As mentioned earlier, a secondary or symptomatic narcolepsy syndrome on occasion results from cerebral trauma, multiple sclerosis, craniopharyngioma, or other tumors of the third ventricle or upper brainstem, or a sarcoid granuloma within the hypothalamus (Servan et al). Furthermore, the nocturnal sleep pattern is altered in narcoleptics, who have frequent body movements and transient awakenings and a decrease in sleep stages 3 and 4 as well as in total sleep. Diagnosis the greatest difficulty in diagnosis relates to the problem of separating narcolepsy from the daytime sleepiness of certain sedentary, obese adults who, if unoccupied, doze readily after meals, while watching television, or in the theater. However, both of these forms of daytime drowsiness are isolated disturbances, lacking the other sleep and motor disturbances that characterize the narcolepsy syndrome. The distinguishing features of narcolepsy are the imperative need for sleep, even under unusual circumstances, and the tendency of the sleep attacks to recur, sometimes abruptly, several times each day. When cataplexy is conjoined with daytime sleepiness, the diagnosis becomes certain. The brief attacks of automatic behavior and amnesia of the narcoleptic must be distinguished from hysterical fugues and complex partial seizures. Excessive daytime somnolence, easily mistaken for idiopathic narcolepsy, may attend sleep apnea syndromes (the most frequent cause), obesity, heart failure, hypothyroidism, excessive use of barbiturates and other anticonvulsants, abuse of alcohol, cerebral trauma, and certain brain tumors. Interestingly, excessive daytime sleepiness is not a frequent part of the chronic fatigue syndrome, although there may be prolonged periods of sleepiness if the illness begins with a mononucleosis-like syndrome. Cataplexy must also be distinguished from syncope, drop attacks (page 329), and atonic seizures; in the latter, consciousness is temporarily abolished. The careful documentation of narcolepsy by laboratory techniques is imperative when the diagnosis is in doubt, in part because of the potential for abuse of stimulant drugs used for treatment. According to some investigators, a reduced level (below 110 pg/mL) of hypocretin in the spinal fluid is virtually diagnostic of narcolepsy in the proper clinical circumstances (see Mignot et al). We would comment, however, that it is rarely necessary to resort to any of these studies in clinically typical cases. The narcolepsy responds best to (1) strategically placed 15- to 20-min naps (during lunch hour, before or after dinner, etc. Until now the drug of choice has been methylphenidate, because of its prompt action and relative lack of side effects. It is usually, given in doses of 10 to 20 mg three times daily on an empty stomach. Alternatively, amphetamine 5 to 10 mg may be given three to five times a day; this is ordinarily well tolerated and does not cause wakefulness at night.
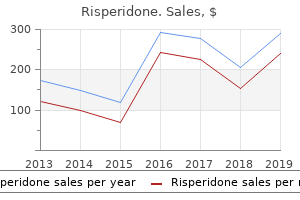
Peduncular hallucinosis may occur in thalamicsubthalamic ischemic lesions, but the exact location of the lesion is unknown. Circular or proximal segment (1) Paramedian arteries (interpeduncular, intercrural, perforating) (2) Quadrigeminal arteries (3) Thalamic arteries (medial and lateral) Regions of vascular supply Substantia nigra, red nucleus, mammillary body, oculomotor nerve, trochlear nerve Quadrigeminal bodies Central nucleus, medial nucleus, ventrolateral nucleus of the thalamus, pulvinar, lateral geniculate body, internal capsule (posterior portion) Epithalamus, thalamus, choroid plexus, pineal gland Tuber cinereum, cerebral peduncle, ventral nuclei of the thalamus, nuclei of the hypothalamus, optic chiasm Hippocampal gyrus, lateral geniculate body, pulvinar, dentate fascia, hippocampus, anterior basal cortex of the temporal lobe, choroid plexus of the temporal horn, trigone, dorsolateral nuclei of the thalamus (4) Medial posterior choroidal arteries (5) Premammillary arteries (of the posterior communicating artery) (6) Peduncular artery (7) Lateral posterior choroidal arteries (anterior and posterior) B. The portion of the posterior cerebral artery giving rise to the interpeduncular branches (the portion between the bifurcation of the basilar artery and the ostium of the posterior communicating artery) is also referred to as the mesencephalic artery or the basilar communicating artery. The thalamoperforate branches (also called paramedian thalamic arteries) arise slightly more distally, near the junction of the posterior cerebral and posterior communicating arteries (P2 segment of the artery) and supply the inferior, medial, and anterior parts of the thalamus. As pointed out by Percheron (whose name is often applied to the largest of these vessels), the arterial configuration of the thalamoperforate arteries varies considerably: in some cases they arise symmetrically, one from each side; in others, both arteries arise from the same posterior cerebral stem, either separately or by a common trunk, which then bifurcates. In the latter case, one posterior cerebral stem supplies the medial thalamic territories on both sides, and an occlusion of this artery or one common paramedian trunk produces a bilateral butterfly-shaped lesion in the medial parts of the diencephalon. The thalamogeniculate branches arise still more distally, opposite the lateral geniculate body, and supply the geniculate body and the central and posterior parts of the thalamus. Medial branches from the posterior cerebral, as it encircles the midbrain, supply the lateral part of the cerebral peduncle, lateral tegmentum and corpora quadrigemina, and pineal gland. Posterior choroidal branches run to the posterosuperior thalamus, choroid plexus, posterior parts of the hippocampus, and psalterium (decussation of fornices). Occlusion of the posterior cerebral artery produces a greater variety of clinical effects than occlusion of any other artery because both the upper brainstem, which is crowded with important structures, and the inferomedial parts of the temporal and occipital lobes lie within its domain. Obviously, the site of the occlusion and the arrangement of the circle of Willis will in large measure determine the location and extent of the resulting infarct. For example, occlusion proximal to the posterior communicating artery may be asymptomatic or have only transitory effects if the collateral flow is adequate from the opposite posterior cerebral vessel. Even distal to the posterior communicating artery, an occlusion may cause relatively little damage if the collateral flow through border-zone collaterals from anterior and middle cerebral arteries is sufficient. In the series of posterior cerebral artery strokes studied by Milandre and coworkers, the causes were in general similar to those of strokes in other vascular territories except that there was a surprisingly high incidence of atherosclerotic occlusion (35 patients) in contrast to cardioembolic types (15 patients). Our experience has differed in that the proportion of presumed embolic occlusions has been far greater than that of other causes. For convenience of exposition, it is helpful to divide the posterior cerebral artery syndromes into three groups: (1) anterior and proximal (involving interpeduncular, thalamic perforant, and thalamogeniculate branches), (2) cortical (inferior temporal and medial occipital), and (3) bilateral. There is both a deep and cutaneous sensory loss, usually severe in degree, of the opposite side of the body, including the trunk and face, sometimes accompanied by a transitory hemiparesis. In some instances there is a dissociated sensory loss- pain and thermal sensation being more affected than touch, vibration, and position- or only one part of the body may be anesthetic. But again, the characteristic feature is sensory loss that includes the entire hemibody up to the midline. After an interval, sensation begins to return, and the patient may then develop pain, paresthesia, and hyperpathia in the affected parts. There may also be distortion of taste, athetotic posturing of the hand, and alteration of mood. Mania and depression have occasionally been observed with infarction of the diencephalon and adjacent structures, but the data are usually incomplete. Central midbrain and subthalamic syndromes are due to occlusion of the interpeduncular branches of the posterior cerebral artery. Syndromes of the paramedian arteries, including the proximal posterior cerebral artery, have as their main feature a third nerve palsy combined with contralateral hemiplegia (Weber syndrome), contralateral ataxic tremor (Benedikt syndrome), or ataxia and hemiparesis (Claude syndrome) as summarized in Table 34-3, page 681. Anteromedial-inferior thalamic syndromes follow occlusion of the thalamoperforant branches. Here the most common effect is an extrapyramidal movement disorder (hemiballismus or hemichoreoathetosis or less often, asterixis). Hemiballismus is usually due to occlusion of a small branch to the subthalamic nucleus (of Luys) or its connections with the pallidum. Occlusion of the paramedian thalamic branch(es) to the mediodorsal thalamic nuclei or to the dominant (left) mediodorsal nucleus is a recognized 3 4 1 2 5 Figure 34-10. Distribution of (1) the anterior cerebral artery, (2) the posterior cerebral artery, (3) the anterior and posterior choroidal arteries, (4) the posterior communicating artery, and (5) the internal carotid artery. Unilateral Cortical Syndromes Occlusion of branches to the temporal and occipital lobes gives rise to a homonymous hemianopia as a result of involvement of the primary visual receptive areas (calcarine or striate cortex) or of the converging geniculocalcarine fibers. It may be incomplete and then involves the upper quadrants of the visual fields more than the lower ones (see Chap.
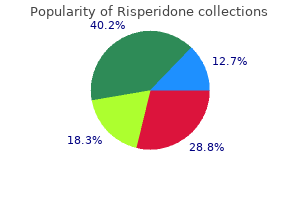
Proprioception was profoundly reduced, but there was no weakness or muscle atrophy, despite generalized areflexia. The sensory deficit attained its maximum severity within a week, after which it stabilized and improved very little. Electrophysiologic studies showed absent or slowed sensory conduction but there were no abnormalities of motor nerve conduction or signs of denervation. Follow-up observations (for up to 5 years) disclosed no neoplastic or immunologic disorder, the usual causes of such a sensory neuronopathy. Lacking pathology, it was assumed, from the permanence of the condition, that sensory neurons were destroyed (sensory neuronopathy). A subsequent series of 42 patients reported by Windebank and colleagues emphasized an asymmetrical and brachial pattern of symptoms in some patients and an initial affection of the face in others. At present, this clinical pattern should be viewed as a syndrome rather than as a disease. Certain drugs and other agents, especially cisplatin and excessive intake of pyridoxine, are also causes of a sensory neuronopathy. In the latter, there is usually some degree of proximal weakness, and the sensory changes do not normally extend to the face and trunk. Acute Uremic Polyneuropathy In addition to the well-known chronic sensory neuropathy associated with chronic renal failure that is discussed later in the chapter, there is a more rapid ("accelerated") process that has not been widely appreciated as a cause of acute and subacute weakness. Most patients in our series were diabetics with stable end-stage renal failure who had been treated by peritoneal dialysis for their long-standing kidney disease (Ropper, 1993). In contrast to the better characterized and less severe chronic uremic neuropathy (page 1149), generalized weakness and distal paresthesias progress in over one or more weeks until a bedbound state is reached. More aggressive dialysis or a change to hemodialysis has little immediate effect, although kidney transplantation is curative. Electrophysiologic studies show some demyelinating features but usually not a conduction block. A few reported cases have been clinically almost indistinguishable from inflammatory demyelinating polyneuropathy, including, in some, a response to plasma exchange or gamma globulin. As with the more Diphtheritic Polyneuropathy (See page 1031) Some of the neurotoxic effects of Corynebacterium diphtheriae and the mode of action of the exotoxin elaborated by the bacillus are described in Chap. Local action of the exotoxin may paralyze pharyngeal and laryngeal muscles (dysphagia, nasal voice) within 1 or 2 weeks after the onset of the infection and shortly thereafter may cause blurring of vision due to paralysis of accommodation, but these and other cranial nerve symptoms may be overlooked. The weakness characteristically involves all extremities at the same time or may descend from arms to legs. After a few days to a week or more, the patient may be unable to stand or walk and occasionally the paralysis is so extensive as to impair respiration. Diphtheritic deaths that occur after the pharyngeal infection has subsided are due to cardiomyopathy or, less often, to severe polyneuropathy with respiratory paralysis. This type of polyneuropathy, now quite rare, should be suspected in the midst of an outbreak of diphtheritic infection, as occurred recently in Russia (Logina and Donaghy). The important pathologic change is one of segmental demyelination without inflammatory reaction of spinal roots, sensory ganglia, and adjacent spinal nerves. Anterior horn cells, axons, peripheral nerves distally, and muscle fibers remain normal (Fisher and Adams). Treatment Diphtheria antitoxin, given within 48 h of the onset of the infection reduces the incidence and severity of neuropathic complications. The prognosis for full recovery is excellent once respiratory paralysis is circumvented. Porphyric Polyneuropathy A severe, rapidly advancing, more or less symmetrical and mainly motor polyneuropathy- often with abdominal pain, psychosis (delirium or confusion), and convulsions- may be a manifestation of acute intermittent porphyria. This type of porphyria is inherited as an autosomal dominant trait and is not associated with cutaneous sensitivity to sunlight. The metabolic defect is in the liver and is marked by increased production and urinary excretion of porphobilinogen and of the porphyrin precursor -amino-levulinic acid. The peripheral and central nervous systems may also be affected in another hepatic type of porphyria (the variegate type). In the latter, the skin is markedly sensitive to light and trauma, and porphyrins are at all times found in the stools. Both of these hepatic forms of porphyria are to be distinguished from the rarer erythropoietic (congenital photosensitive) porphyria, in which the nervous system is not affected.
Diseases
Pica (the compulsive ingestion of nonnutritive substances) is a problem between ages 2 and 4 years of age but is also seen in normal neglected children. The parents of a large proportion of children with all of these abnormal behaviors fall into the lowest segment of the population socially and economically; in other words, the parents may lack the competence to maintain stable homes and to find work, for which reason abandonment, neglect, and child abuse are frequent in this group. The majority of children with deviant behavior need to be placed in special classes or schools, and special measures must be taken to reduce the tendency to truancy, sociopathy, and criminality. An endless debate is centered on matters of causation- whether these categories of mild retardation are products of a faulty genetic influence, which prevents successful competition and adaptation, or of societal discrimination and lack of training and education coupled with the effects of malnutrition, infections, or other exogenous factors. Surely both environmental and genetic factors are at work, although the relative importance of each has proved difficult to measure (Moser et al). As mentioned earlier, a pathologic basis for most cases of mild mental retardation has not been established. No visible lesions have been discerned in the brains of this group, unlike those of the severely retarded (pathologic) group, in which malformations and a variety of destructive lesions are obvious in all but 5 to 10 percent of cases. Admittedly, the brains of some of these individuals are about 10 percent underweight, but one cannot at present interpret what this means. It is certain that new methodologies, perhaps relating to neuronal connectivity, will be needed if the cerebra of the subnormal extreme of the general population are to be differentiated from normals. Differences might be expected in terms of the number of neurons in thalamic nuclei and cortex, in dendriticaxonal connectivity, or in synaptic surfaces, elements that are not being assayed by the conventional techniques of tissue neuropathology. The observations of Huttenlocher, who found a marked sparsity of dendritic arborization in Golgi-Cox preparations, and of Purpura, who found an absence of short, thick spines on dendrites of cortical neurons and other abnormalities of dendritic spines, are the first steps in this direction. Renpenning and colleagues reported a series of 21 mentally retarded males in three generations of a Canadian family, all free of any congenital malformations and with normal head size, and Turner and coworkers have described a similar Australian series (page 888). The fragile-X syndrome (page 889) is another in this group, predominating in males and accounting for about 10 percent of all male retardates. Other X-linked forms of mental retardation that have few or no dysmorphic features besides Renpenning and fragile-X syndromes include the Partington, Lowe, Lesch-Nyhan, and Menkes syndromes and adrenoleukodystrophy, each with special characteristics in addition to mental retardation, as discussed in Chaps. Numerous other X-linked retardation syndromes with accompanying neurologic anomalies have been delineated; for example, the one due to a mutation in the oligophrenin gene, in which there is epilepsy, and another involving cerebellar hypoplasia. Diagnosis Infants should be considered at risk for mental subnormality when there is a family history of mental deficiency, low birth weight in relation to the length of gestation (small-for-date babies), marked prematurity, maternal infection early in pregnancy (especially rubella), and toxemia of pregnancy. In the first few months of life, certain of the behavioral characteristics described above are of value in predicting mental retardation. Prechtl and associates have found that a low Apgar score (especially at 5 min after delivery, Table 28-3), flaccidity, underactivity, and asymmetrical neurologic signs are the earliest indices of subnormality in the infant. Slow habituation of orienting reactions to novel auditory and visual stimuli and the presence of "fine motor deficits" (as previously discussed under "Delays in Motor Development") are other early warnings of mental retardation. In the first year or two of life, suspicion of mental retardation is based largely on clinical impression, but it should always be validated by psychometric procedures. For testing of preschool children, the Wechsler Preschool and Primary Scale of Intelligence is used, and for school-age children, the Wechsler Intelligence Scale for Children is preferred. In general, however, normal scores for age on any of these tests essentially eliminate mental retardation as a cause of poor school achievement and learning disabilities; special cognitive defects may, however, be revealed by low scores on particular subtests. Retarded children not only have low scores but exhibit more scatter of subtest scores. Also, like demented adults, they generally achieve greater success with performance than with verbal items. It is essential that the physician know the conditions of testing, for poor scores may be due to fright, inadequate motivation, lapses in attention, dyslexia, or a subtle auditory or visual defect rather than a developmental lag. Is there one domain of faulty psychologic function- such as failure of learning, inattentiveness, or faulty perception- that underlies all forms of mental retardation? Or are there several domains, differing from one case to another or one disease to another? Only by the most innovative and sophisticated neuropsychologic studies will answers to such questions be obtained. Presumably this is due to a greater degree of immaturity of the cerebrum at any given age. In the diagnosis of milder grades of retardation, always to be considered are the possible effects of severe malnutrition, neglect and deprivation, chronic systemic disease, iodine deficiency, impaired hearing and vision, and possibly childhood psychosis. Of particular importance is the differentiation of a group of patients who are normal for a variable period after birth and then manifest a progressive decline from disease of the nervous system. This type of disorder is representative of the group of hereditary metabolic and degenerative diseases discussed in Chap.
The latter, referred to as paraneoplastic disorders, include polyneuropathy (especially with carcinoma of the lung), polymyositis, cerebellar degeneration (ovarian and other carcinomas and Hodgkin disease), necrotizing myelopathy (rare), and certain cerebral disorders (progressive multifocal leukoencephalopathy and "limbic encephalitis"). These paraneoplastic syndromes are discussed further on, under "Remote Effects of Neoplasia on the Nervous System. These mental symptoms usually arise on the basis of systemic metabolic disturbances (hypercalcemia in particular), drugs, and psychologic reactions, some of which have yet to be clearly delineated. Problems of this type were noted in a high percentage of cancer patients seen in consultation at the Memorial Sloan-Kettering Cancer Center (Clouston et al) and in our own patients. Treatment the treatment of secondary (metastatic) tumors of the nervous system is undergoing change. Corticosteroids produce prompt improvement, but sustained use is restricted by their many side effects and eventual loss of efficacy. Most patients also temporarily benefit from the use of whole-brain irradiation, usually administered over a 2-week period, in 10 doses of 300 cGy each. Patchell and coworkers have shown that survival and the interval between treatment and recurrence are longer and that the quality of life is better in patients treated in this way than in comparable patients treated with wholebrain radiation alone. Single or dual metastases from renal cell cancer, melanoma, and adenocarcinoma of the gastrointestinal tract lend themselves best to surgical removal, sometimes repeatedly. Several clinical trials in patients with small-cell carcinoma of the lung suggest that prophylactic irradiation of the neuraxis decreases the occurrence of metastases but does not prolong survival (Nugent et al). Also, there is increasing evidence that some metastatic brain tumors are quite sensitive to certain chemotherapeutic agents, especially if the primary tumor is also sensitive. Intrathecal and intraventricular chemotherapy are not thought to be of value in the treatment of parenchymal metastases. Some tentative evidence favors their use, but- as mentioned earlier- the incidence of skin reactions is increased when phenytoin is employed and radiation is given. Other studies, some well controlled, have shown no benefit in preventing a first seizure in patients with a primary or secondary brain tumor. The average period of survival, even with therapy, is about 6 months, but it varies widely and is dominated by the extent of other systemic metastases. Between 15 and 30 percent of patients live for a year and 5 to 10 percent for 2 years; with certain radiosensitive tumors (lymphoma, testicular carcinoma, choriocarcinoma, some breast cancers), survival can be much longer. Patients with bone metastases tend to live longer than those with parenchymatous and meningeal metastases. Meningeal Carcinomatosis ("Carcinomatous Meningitis") Widespread dissemination of tumor cells throughout the meninges and ventricles, a special form of metastatic cancer, has been the pattern in about 5 percent of cases of adenocarcinoma of breast, lung, and gastrointestinal tract; melanoma; childhood leukemia; and systemic lymphoma. With certain carcinomas, notably gastric in our experience, it may be the first manifestation of a neoplastic illness, although more often the primary tumor has been present and is under treatment. Only a small number have an uncomplicated menigneal syndrome of headache, nausea, and meningismus, but these features develop late in the course of many cases. Focal neurologic signs and seizures may be associated, and somewhat fewer than half the patients develop hydrocephalus. It may cause a painful or painless polyradiculopathy and simulate a polyneuropathy; it has several times deceived us into considering the diagnosis of an inflammatory polyneuropathy. The combination of a cranial neuropathy, such as unilateral facial weakness, hearing loss or ocular motor palsy, with bilateral asymmetrical limb weakness is particularly suggestive. The evolution in all these syndromes is generally subacute over weeks with a more rapid phase as the illness progresses. These markers are most likely to be abnormal in hematologic malignancies but may also be altered in some cases of intracranial infection and parenchymal metastases (Kaplan et al). In a few of the cases of meningeal carcinomatosis, there are also parenchymal brain metastases. Also known is a rare primary malignant melanoma of the meninges that acts in a similar way to carcinomatous meningitis. The prognosis for this condition is quite poor (lymphomatous infiltration is an exception); seldom does the patient survive more than 1 to 3 months, perhaps longer by several weeks if treatment is successful. An encephalopathy due to widespread infiltration of the cerebral meninges is a particularly malevolent sign.
More severe rashes may develop, sometimes taking the form of erythema multiforme and Stevens-Johnson syndrome, or even toxic epidermal necrolysis. A rare hypersensitivity syndrome is one of high fever, rash, lymphadenopathy, and pharyngitis. If any of these reactions require that one of the aromatic drugs be replaced, valproate, gabapentin, topiramate, or levetiracetam are reasonable substitutes, depending, of course, on the nature of the seizures. Treatment of Seizures in the Neonate Treatment of the special types of convulsions in the neonatal period and in infancy and childhood is discussed by Fenichel and by Volpe. Probably the form of epilepsy that is most difficult to treat is the childhood Lennox-Gastaut syndrome. Some of these patients have as many as 50 or more seizures per day, and every combination of anticonvulsant medications may have no effect. Valproic acid (900 to 2400 mg/day) will reduce the frequency of spells in approximately half the cases. The newer drugs- lamotrigine, topiramate, vigabatrin- are each beneficial in about 25 percent of cases. Most patients who die of epilepsy do so because of uncontrolled seizures of this type, complicated by the effects of the underlying illness or an injury sustained as a result of a seizure. Rising temperature, acidosis, hypotension, and renal failure from myoglobinuria is a sequence of life-threatening events that may be encountered in cases of status epilepticus. Prolonged convulsive status (for longer than 30 min) also carries a risk of serious neurologic sequelae ("epileptic encephalopathy"). With regard to acute medical complications, from time to time a case of neurogenic pulmonary edema is encountered during or just after the convulsions, and some patients may become extremely hypertensive, then making it difficult to distinguish the syndrome from hypertensive encephalopathy. Treatment (Table 16-9) the many regimens that have been proposed for the treatment of status attest to the fact that no one of them is altogether satisfactory and none is clearly superior (Treiman et al). A large-bore intravenous line is inserted; blood is drawn for glucose, blood urea nitrogen, electrolytes, and a metabolic and drug screen. A normal saline infusion is begun and a bolus of glucose is given (with thiamine if malnutrition and alcoholism are factors). To rapidly suppress the seizures, diazepam is given intravenously at a rate of about 2 mg/min until the seizures stop or a total of 20 mg has been given. Immediately thereafter, a loading dose (15 to 18 mg/kg) of phenytoin is administered by vein at a rate of less than 50 mg/min. More rapid administration risks hypotension and heart block; it is therefore recommended that the blood pressure and electrocardiogram be monitored during the infusion. Phenytoin must be given through a freely running line with normal saline (it precipitates in other fluids) and should not be injected intramuscularly. A large study by Treiman and colleagues has demonstrated the superiority of using lorazepam instead of phenytoin as the first drug to control status, but this is not surprising considering the longer latency of action of phenytoin. Alldredge and colleagues have shown that diazepines can even be administered by paramedical workers with good effect in status epilepticus, terminating the seizures in about half of these patients. Nonetheless, a long-acting anticonvulsant such as phenytoin is given immediately after diazepam has controlled the initial seizures. An alternative is the water-soluble drug fosphenytoin, which is administered in the same doses as phenytoin but can be injected at twice the maximum rate. Moreover, it can be given intramuscularly in cases where venous access is difficult. However, the delay in hepatic conversion of fosphenytoin to active phenytoin makes the latency of clinical effect approximately the same for both drugs. In an epileptic patient known to be taking anticonvulsants chronically but in whom the serum level of drug is unknown, it is probably best to administer the full recommended dose of phenytoin or fosphenytoin. If it can be established that the serum phenytoin is above 10 mg/mL, a lower loading dose is advisable. If this fails to suppress the seizures and status has persisted for 20 to 30 min, an endotracheal tube should be inserted and O2 administered. Several approaches have been suggested to control status that persists after these efforts. The conventional and still dependable one is infusion of either thiopental, starting with 5 mg/kg, or phenobarbital, at a rate of 100 mg/min until the seizures stop or a total dose of 20 mg/kg is reached. In our experience, a long period of stupor must be anticipated after seizure control is obtained, but some epileptologists still prefer this as the initial treatment.
We would refer to this state as periventricular interstitial edema in association with tension hydrocephalus. The use of high-potency glucocorticosteroids has a beneficial effect on the vasogenic edema associated with tumors, both primary and metastatic, sometimes beginning within hours. Probably these steroids act directly on the endothelial cells, reducing their permeability. Steroids also shrink normal brain tissue, thus reducing overall intracranial pressure. In addition, drugs such as dexamethasone reduce the vasogenic edema associated with brain abscess and head injury, but their usefulness in cases of large cerebral infarctions, contusions, and hemorrhage is less clear. Possibly the swelling of necrotic tissue is reduced; however, there is no evidence that cytotoxic or cellular edema responds to administration of glucocorticoids. For patients with brain tumor, it is common practice to use doses of dexamethasone of approximately 4 mg every 6 h, or the equivalent dose of methyprednisolone (Solu-Medrol), while a few patients require a rigid schedule; otherwise, a dose with meals and at bedtime usually suffices to suppress headache and focal tumor signs. In patients with large tumors and marked secondary edema, further benefit is sometimes achieved by the administration of extremely high doses of dexamethasone, to a total of 100 mg per day or more. Always to be kept in mind are the potentially serious side effects of sustained steroid administration, even at standard dose levels. Therefore the schedule should be carefully titrated to the desired clinical effect. It is also recognized that these drugs interfere with the metabolism of certain anticonvulsants commonly used in brain tumor patients. In patients who have brain edema and who require intravenous fluids, solutions containing water ("free water") not matched by equivalent amounts of sodium should be avoided. Mannitol is the most widely used; a 25% solution is administered parenterally in a dose of 0. Urea is used less often and glycerol is not much favored in the United States because of its high caloric content, but it is used in Europe, largely because it can be taken orally on an outpatient basis. A single administration of these solutes has only a short-lived effect, a matter of several hours or less as the brain extracellular space reaches an equilibrium concentration, but repeated use on a regular schedule can lead to a reduction in headache and stabilization of some of the deleterious effects of a mass. Aside from a diuresis, which may raise serum osmolality, highly permeable solutes such as glucose do little to reduce brain volume, since they do not create an osmolar gradient that moves water from the brain to the vasculature. Furthermore, with repeated administration of hyperosmolar solutions such as mannitol or with diuretics, the brain gradually increases its osmolality- the result of added intracellular solute; these agents are therefore not suitable for long-term use. The notion that hyperosmolar agents might exaggerate tissue shifts by shrinking normal brain tissue has not been substantiated. The net effect of hyperosmolar therapy is reflected roughly by the degree of hyperosmolarity and hypernatremia that is attained. The main aspects of this problem, particularly the coma-producing mechanisms, have been considered on page 310. The pressure from a mass within any one dural compartment causes shifts or herniations of brain tissue to an adjacent compartment where the pressure is lower. Herniation of swollen brain through an opening in the calvarium, in relation to craniocerebral injury or operation, is yet another (transcalvarial) type. As mentioned, the transtentorial herniations relating primarily to coma were discussed in Chap. The writings of Meyer, Jefferson, and Kernohan may be consulted for the early descriptions of the herniations. Subfalcial herniation, in which the cingulate gyrus is pushed under the falx, occurs frequently, but little is known of its clinical manifestations except that there is often occlusion of an anterior cerebral artery and frontal lobe infarction. The displacement may be bilateral or, in the case of a onesided cerebellar lesion, ipsilateral. Cushing considered the typical signs of cerebellar herniation to be episodic tonic extension and arching of the neck and back and extension and internal rotation of the limbs, with respiratory disturbances, cardiac irregularity (bradycardia or tachycardia), and loss of consciousness.
References: